Tags
Aging, arthritis, health, joint-pain, knee-pain, Lifestyle, optimal health, osteoarthritis, Vitality
A little over two years ago, I hurt my knee. I was doing some vigorous aerobic workout style dancing. I might have twisted my right knee and it started to hurt really badly. I thought it would be fine in a couple of weeks by giving it the usual TLC. But it took over two years to heal it. And it turned out to be quite an opportunity to learn.
Whenever I talk to my contemporaries, the topic of knee pain comes up frequently. So, I thought I would share here my journey of healing my knee pain and more importantly the resources I found useful. Trust others will find this information useful.
In this Part 1 of this series of blog posts, I share different resources for diagnose and fix the structural issues with my knee.
History and Background
You see I have been dealing with knee pain off and on for a long time. About 30 years ago, I took up the goal of running a marathon. I started the training. Ran my first 5K and then my right knee started hurting when I would run. Could not figure out how to run pain free. So, that was the end of my marathon running goal.
Since that episode, over the last thirty years, I have been working on bringing my knee functionally to 100%, judging by the capacity and capability of my left knee. It is still not there 100%, but it is the closest it has come to that goal in thirty years.
Resource #1 – Orthopedic Doctors
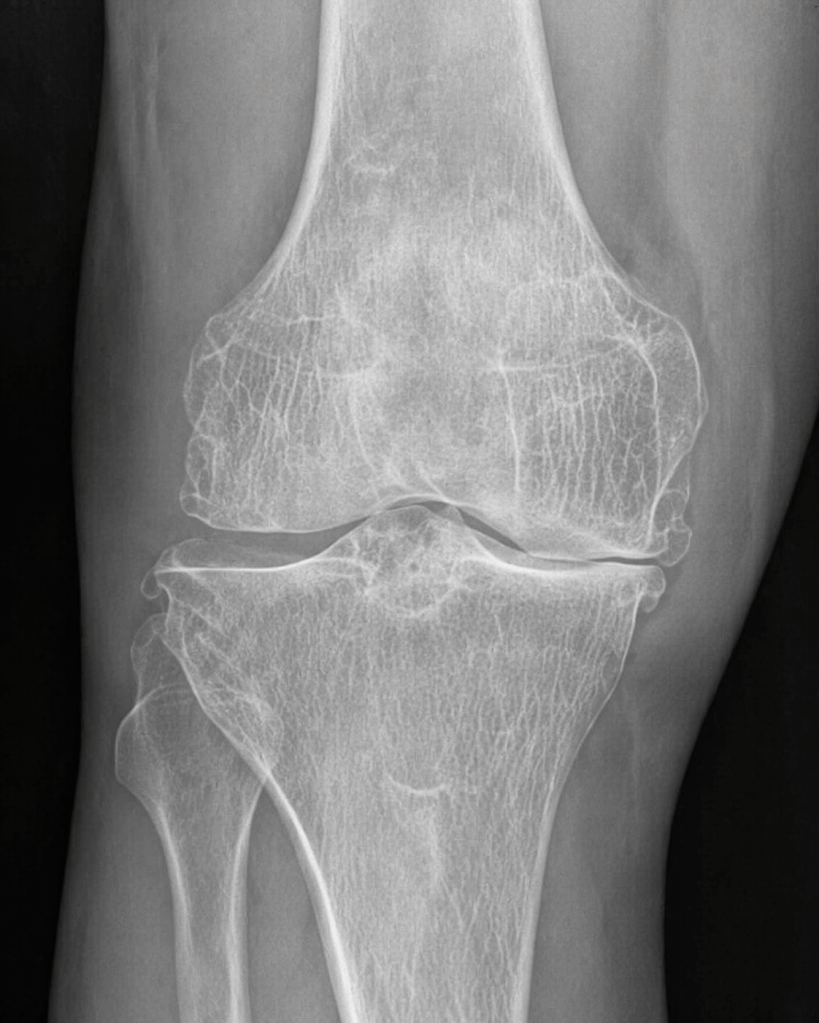
My first stop was to get my knee checked out by an orthopedic doctor. I even picked a practice specializing in Sports Medicine. They did a quick X-ray, showed me the picture and pointed out that I had a mild case of osteoarthritis in my knee.
So, what do I do then? I was told not to run. And, if I was to run, maybe use a knee brace. I bought a brace. Tried running with it. Did not really work.
Over the years, the pain went away but it did not really allow me to run. However, I became comfortable with a variety of activities, jumping rope, skiing, rollerblading and so on.
And this time around, which is about two years ago, another trip to the orthopedic knee specialist. A quick X-ray, was showed the picture and told that now I had mild-to-moderate osteoarthritis. Nothing broken, nothing torn. This time, my options were: a) Steroid injection in the knee, b) Injecting gel, if I got permission from the insurance company, c) Take ibuprofen, or d) Do nothing. Learned that the steroid injection was not simply to relieve the pain but was also therapeutic, since it would relieve the inflammation. So, I chose to get the injection.
Other options offered at the orthopedic specialist’s office are arthroscopic surgery and knee replacement surgery.
Orthoscopic surgery was very popular up to a decade or so ago. These have lately fallen out of favor. Clinical trials done during the last few years have shown that orthoscopic surgery is no more effective than the placebo in the form of sham surgery.
Knee Replacement is an option only when the pain is so severe that you can no longer tolerate the pain whether awake or sleeping since the cartilage has pretty much worn out.
My experience – Orthopedic specialists are a great resource to find out if I broke anything or tore anything for which they have solutions. For osteoarthritis, other than a steroid injection basically, wait until the knee is ready for replacement.
Resource #2 – Hyaluronic Acid
A quick take on hyaluronic acid from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4469223/
“…Viscosupplementation with intra-articular hyaluronic acid is a treatment option in knee OA that is included in the professional guidelines for treatment of this joint disease, but potentially should apply to all synovial joints in order to reduce pain and improve joint lubrication. Exogenous HA can enhance chondrocyte HA synthesis, prevent the degradation of cartilage and promote its regeneration. Moreover it can reduce the production of proinflammatory mediators and matrix metalloproteinases involved in OA pathogenesis. This mini review highlights the evidence of hyaluronic acid in reducing osteoarthritis symptoms and structural damage, as well as its ability to delay prosthetic surgery. Viscosupplementation should be considered as a long-term therapy.”
Basically, hyaluronic acid is a gel that if injected into the knee joint improves joint lubrication, reduces inflammation and may also regenerate cartilage improving the structure of the joint. Treatment may have to be repeated over time as a long-term therapy.
Typically, insurance companies do not cover this therapy. It is known to relieve knee pain and improve joint functions. Some orthopedic specialists may offer it. But mostly these are offered by those doctors practicing alternative therapies, e.g., functional doctors, chiropractors or doctors of osteopathy.
Resource #3 – Platelet Rich Plasma (PRP) Therapy
PRP therapy for osteoarthritis of the knee works by injecting platelet-rich blood into the area surrounding the knee to help reverse existing tissue damage. Blood is comprised of four components. Most of your blood is liquid, known as plasma. The other three components are platelets, white blood cells, and red blood cells.
Platelets play a key role in the clotting of the blood. They also contain growth factors that could help tissues repair themselves by causing new cells to form.
PRP Therapy involves taking blood from the veins, about the quantity typically used for blood tests. They spin it to separate plasma and platelets from the red blood cells. They then inject plasma into the joint, where the cartilage might be damaged, typically where it hurts to touch and/or where inflammation in the joint is.
PRP is still not mainstream as a standard of care. Here is one article, comparting results of various studies on PRP And Hyaluronic Acid, https://pubmed.ncbi.nlm.nih.gov/34785294/ . The bottom line from this study is: Patients undergoing treatment for hip or knee OA with either PRP or HA injections can expect to experience similarly beneficial short-term clinical outcomes.
My experience – I underwent three different applications of PRP. And found those to be beneficial.
Resource #4 – Stem cell Therapy
Stem Cell Therapy procedures are non-surgical injection-based procedures for people suffering from knee pain due to common injuries to the knee Meniscus, ACL, MCL, and other structures, or who are experiencing degenerative conditions such as Osteoarthritis. These procedures utilize concentrated repair cells that are obtained from your own bone marrow or blood to promote your body’s own natural ability to heal.
I visited folks at StemCellArts to see what they could do for my knee. The procedures they perform are done by orthopedic doctors who have a lot of experience and have developed specific protocols. However, the procedure tends to be quite expensive and is also quite involved, especially the part about extracting stem cells from bone marrow and culturing those cells.
Later, I also learned about the stem cells that are now harvested from umbilical cords, packaged and then distributed for doctors to use. This approach seemed to be rather inexpensive compared to using bone marrow. I underwent this procedure and found it to be quite helpful. In fact, a few months after the stem cell procedure, I asked the doctor if he would recommend repeating it. He recommended that once the joint is seeded with the stem cell, it was more helpful to do a PRP procedure to provide the joint more “fertilizer” in the form of growth factors. That is why I ended up doing the third PRP procedure.
My experience – My knee used to be tender to touch on the left side of the knee, where X-rays showed cartilage had eroded. After the stem cell and PRP procedures the tenderness and accompanying pain totally went away.
Bottom Line:
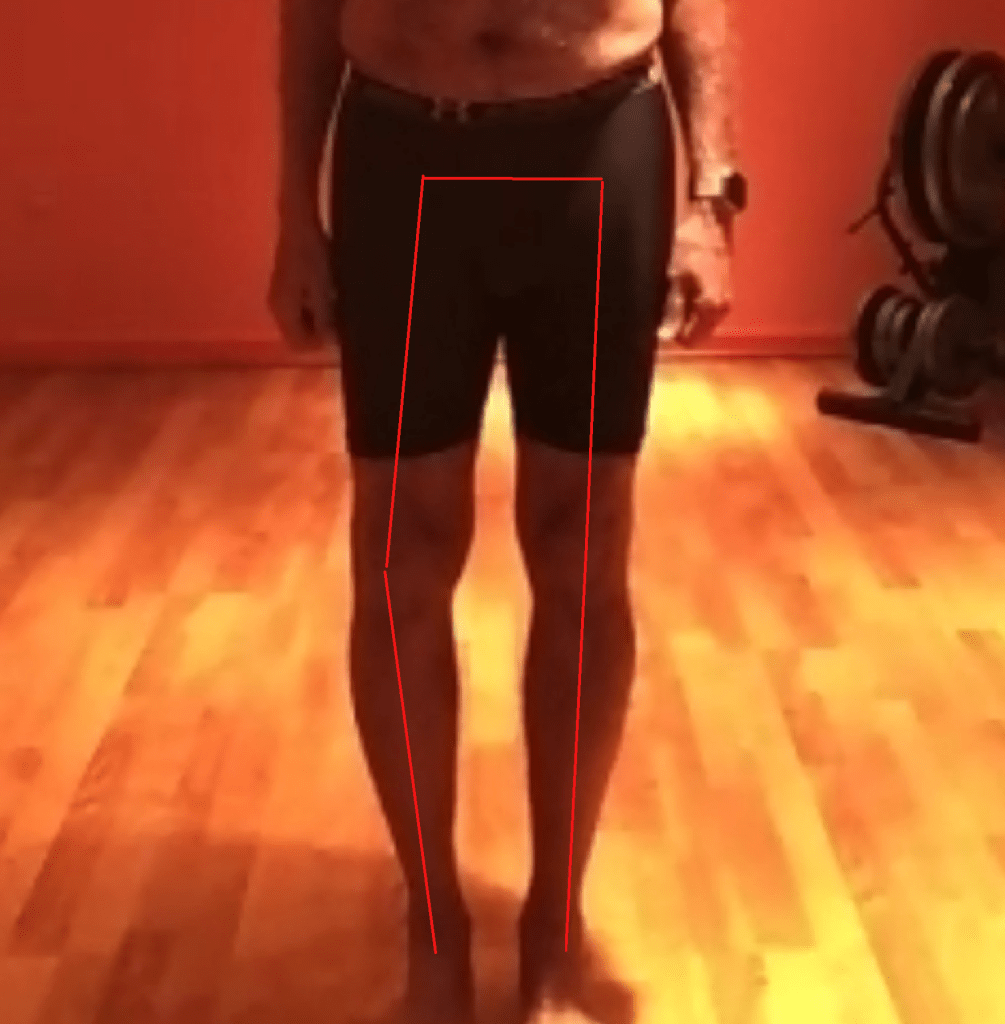
From my research and experience, I have found that it is important to find out what is the underlying structural issue for knee pain. It could be osteoarthritis, meniscus tears, tendon & ligament tears, overuse injuries or some other condition. In my case, it was osteoarthritis, clearly showing eroded cartilage in certain part of the knee joint. The resources that were useful to diagnose and repair the structural damage were:
- Visit to the Orthopedic surgeon and imaging
- Steroid injection for relieving inflammation.
- Alternatively, ibuprofen for relieving inflammation.
- Hyaluronic acid or PRP treatment for joint lubrication and repair.
- Stem Cell therapy for repair or regeneration.
Of course, this is not medical advice, and you should check with a medical doctor about your specific situation.
What are your thoughts or experience on this subject?
Would love to hear from you and learn from you.
Please click on Comment to leave your comments or question so others can benefit from your input.









 As I mentioned in my previous post #58, I consider Michael Greger’s website
As I mentioned in my previous post #58, I consider Michael Greger’s website  In my blog post #9 – When it comes to health, vitality and aging what is really possible?, I had discussed the book, Prevent and Reverse Hearth Disease by Caldwell B. Esselstyn, Jr. M.D. In this book, Dr. Fuhrman’s has updated research on preventing and reversing heart disease. Case studies are mind blowing. He not only gives research but actually prescription on what you should actually eat and even very specific meal plans. Dr. Furhman promises his patients to let him decide what they eat for six weeks and then based on the result they can then decide what to eat. Most of them become converts to his prescription of nutrition after seeing the results.
In my blog post #9 – When it comes to health, vitality and aging what is really possible?, I had discussed the book, Prevent and Reverse Hearth Disease by Caldwell B. Esselstyn, Jr. M.D. In this book, Dr. Fuhrman’s has updated research on preventing and reversing heart disease. Case studies are mind blowing. He not only gives research but actually prescription on what you should actually eat and even very specific meal plans. Dr. Furhman promises his patients to let him decide what they eat for six weeks and then based on the result they can then decide what to eat. Most of them become converts to his prescription of nutrition after seeing the results. I did a series for posts #51-#54 on How to Optimize Your Immune System. In this book, Dr. Fuhrman offers a lot more research and very practical ways to build immunity so your body can fight whatever comes its way – not only flues and colds, but also other infections and even cancer. Cancer after-all is just DNA mutation that body fights all day long. Only when our immune system is NOT capable of handling the mutated DNA, it starts to take over the organs unchecked. Again, the book includes nutrition meal plans, recipes to put into practice his philosophy – not just eat food that is packed with desired micro-nutrients, but eat a lot of it.
I did a series for posts #51-#54 on How to Optimize Your Immune System. In this book, Dr. Fuhrman offers a lot more research and very practical ways to build immunity so your body can fight whatever comes its way – not only flues and colds, but also other infections and even cancer. Cancer after-all is just DNA mutation that body fights all day long. Only when our immune system is NOT capable of handling the mutated DNA, it starts to take over the organs unchecked. Again, the book includes nutrition meal plans, recipes to put into practice his philosophy – not just eat food that is packed with desired micro-nutrients, but eat a lot of it. In blog post #50, I discussed how to optimize your health by maximizing your telomeres. Elizabeth Blackburh received Nobel Prize for her research in telomeres. Telomeres are the end-caps at the ends of our DNA strands like little plastic wraps at the end of shoe laces. If the little plastic wraps are damaged shoe laces become useless, so is the case with the DNA. The length of telomeres correlate with the remaining lifespan. Dr. Blackburn shares the latest research in lay-person language and shares the different methods by which we can increase the length of our telomeres. Reading this book, it should not come as surprise to you that the lifestyle choices I discussed in my Post #59, all help increase the lengths of your telomeres.
In blog post #50, I discussed how to optimize your health by maximizing your telomeres. Elizabeth Blackburh received Nobel Prize for her research in telomeres. Telomeres are the end-caps at the ends of our DNA strands like little plastic wraps at the end of shoe laces. If the little plastic wraps are damaged shoe laces become useless, so is the case with the DNA. The length of telomeres correlate with the remaining lifespan. Dr. Blackburn shares the latest research in lay-person language and shares the different methods by which we can increase the length of our telomeres. Reading this book, it should not come as surprise to you that the lifestyle choices I discussed in my Post #59, all help increase the lengths of your telomeres. Time did a fantastic job in summarizing the latest in science of exercise in this special Time Magazine publication. If you needed any further evidence how exercise impacts health and lifespan, I believe this publication will deliver, without having to read some big tome. The issue spans many diverse topics: cardio vs. weights, high intensity interval training, running, swimming, yoga and other exercise modalities.
Time did a fantastic job in summarizing the latest in science of exercise in this special Time Magazine publication. If you needed any further evidence how exercise impacts health and lifespan, I believe this publication will deliver, without having to read some big tome. The issue spans many diverse topics: cardio vs. weights, high intensity interval training, running, swimming, yoga and other exercise modalities. In my blog post #17 – Is meditation an effective antidote to stress, I talk about Transcendental Meditation or TM as a very effective and well-researched means for combating stress. Science of Being and Art of Living is book compiled based on lectures by Maharishi Mahesh, who introduced TM to the West. He also founded the TM movement that has established TM Centers pretty much in all major cities throughout the world. While first part of the book serves as evidence and motivation for TM, the later parts are more for the practitioners and advanced students of TM and Yoga.
In my blog post #17 – Is meditation an effective antidote to stress, I talk about Transcendental Meditation or TM as a very effective and well-researched means for combating stress. Science of Being and Art of Living is book compiled based on lectures by Maharishi Mahesh, who introduced TM to the West. He also founded the TM movement that has established TM Centers pretty much in all major cities throughout the world. While first part of the book serves as evidence and motivation for TM, the later parts are more for the practitioners and advanced students of TM and Yoga. A few months ago, I got a chance to meet and attend a work shop by Dr. Levy, who has spent all his life building bridges between Western medicine and Eastern philosophies of yoga and meditation. Dr. Levy talks about how to prevent and reverse heart diseases by tackling the most insidious of the issues that impact heart health, i.e., Stress. This manual is accompanied by CDs on which you will find and can actually use his hypnosis techniques for relieving stress and anxiety.
A few months ago, I got a chance to meet and attend a work shop by Dr. Levy, who has spent all his life building bridges between Western medicine and Eastern philosophies of yoga and meditation. Dr. Levy talks about how to prevent and reverse heart diseases by tackling the most insidious of the issues that impact heart health, i.e., Stress. This manual is accompanied by CDs on which you will find and can actually use his hypnosis techniques for relieving stress and anxiety. In this more recent publication, The Happiness Sutra, Dr. Levy further delves into the four different types of stresses humans face and how best to deal with all four types of stresses. This book also has a CD that you can listen to to get the benefit of Dr. Levy’s hypnosis methods for relieving stress.
In this more recent publication, The Happiness Sutra, Dr. Levy further delves into the four different types of stresses humans face and how best to deal with all four types of stresses. This book also has a CD that you can listen to to get the benefit of Dr. Levy’s hypnosis methods for relieving stress. Lissa Rankin, M.D.’s book Mind Over Medicine is a great case study of extreme stress brought on modern living and by our current medical system. Dr. Rankin, a practicing OB GYN, quit her practice of medicine because of the numerous health and personal issues brought on by stress from her profession. She eventually found ways to heal herself and then learned to apply her new found knowledge to become a true healer, without becoming slave to the medical system.
Lissa Rankin, M.D.’s book Mind Over Medicine is a great case study of extreme stress brought on modern living and by our current medical system. Dr. Rankin, a practicing OB GYN, quit her practice of medicine because of the numerous health and personal issues brought on by stress from her profession. She eventually found ways to heal herself and then learned to apply her new found knowledge to become a true healer, without becoming slave to the medical system.